Mortality with Meep: Comparing COVID-19 with Historical Mortality and Prior Pandemics
Yes, COVID-19 shows serious mortality increases
My usual way to do a post is to go chronologically, building up from a base, and working toward a conclusion.
I’m going to give you my conclusions first, and then, if you’re interested, you can read how I got there.
COVID-19 is a serious mortality event
I have shown this before, but COVID-19 is a serious increase in U.S. mortality in 2020 (and we’ll see if it continues into 2021 and farther). There are some indications that the nastiest, most fatal wave passed in the spring, and I’ll link to that evidence in my next COVID round-up post.
Here is the first graph, showing my minimal projection for 2020 deaths versus U.S. historical mortality, broken out by age:
The “minimal” projection assumes excess deaths stopped on October 17, 2020 [they didn’t], and the reason I used this assumption is to show COVID-mortality skeptics that yes, that is quite the bump-up in mortality. That’s about an 8% jump from 2018 to 2020, and that’s my lower bound estimate for 2020.
My “best guess” is more like a 10% increase from 2018 to 2020. [The reason I exclude 2019 is that I don’t have those death counts at all… the CDC usually releases such data over a year later, because it takes time to get it all in good order.] I will be using my “best guess” projection later, which doesn’t incorporate the still-catastrophic projections we sometimes hear from interested groups. The minimal projection is unlikely – it includes all the deaths already counted for 2020 and just assumes normal mortality resumes after that.
Comparing 2020 death projections to 2018
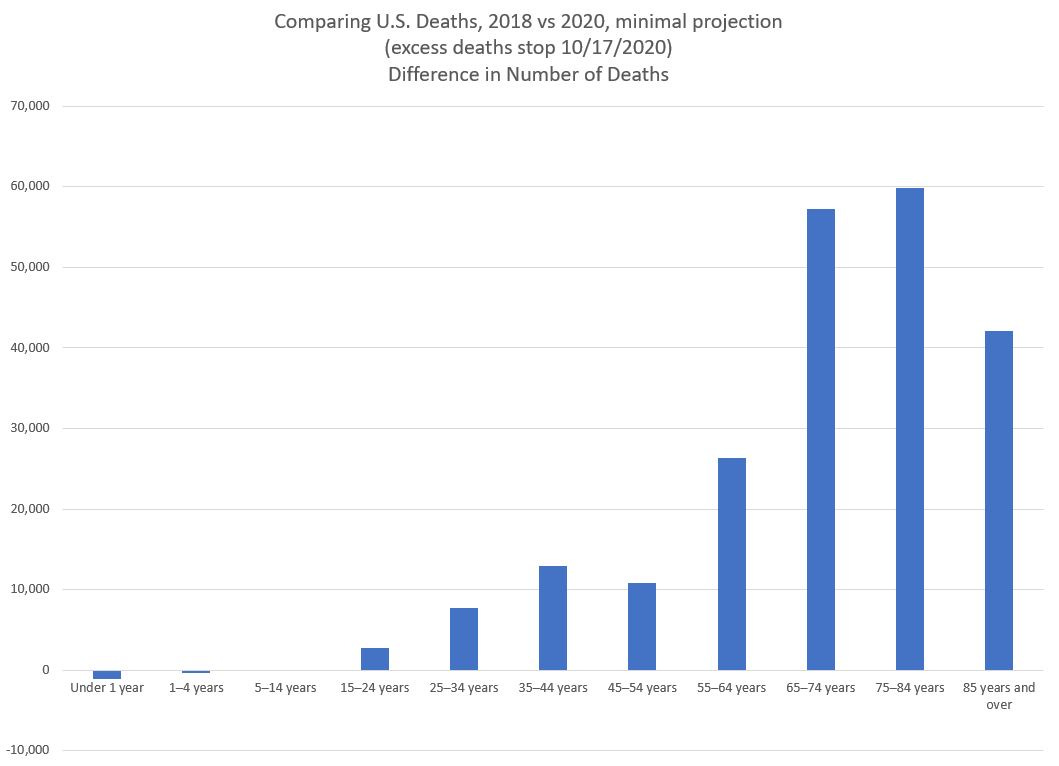
Here is the second graph, showing the 2018-to-2020 increase in deaths by age group (again, my minimal projection):
Note that the under-age-15 grouping may also be influenced by birth patterns (fewer births lead to fewer deaths, just by counting.) We really should be comparing death rates – but rates are more difficult to develop. I will look at those in a future post.
I really don’t like the look of the spike in age 35-44 deaths. I will need to look at the data – it overlaps with the “baby bust” group of Gen X, and very few people die in that age group in normal years. But, if there are increases in drug overdoses and suicides, that is about the age range I would expect to see the largest effects (because other things start killing people more at older ages). If we look at the difference in the number of deaths in the minimal projection:
The large percentage differences at young ages come from such a very low death rate for those age groups. So only a difference of 13,000 deaths leads to an over 15% difference in the count of deaths year-over-year for those age 35-44.
The small number of deaths fewer for children in 2020 is likely coming from fewer car accidents in which they’re involved (no school or after-school activities to be shuttled around) and fewer drownings (pools and beaches closed). Accidental causes of death are the number one killer of small children, and among accidental causes, car accidents and drowning are tops for kids.
Historical trend in death count increases/decreases
Over long periods, death rates are the more relevant comparison, of course. The population base and age structure of the U.S. population were very different in 1950 compared to 2020, after all.
However, the year-over-year percentage change can show the effects of fleeting events, such as pandemics. The population size, at least in the U.S. post-1930, did not increase much in a single year. Yes, there is immigration, but again, that will come out in longer-term trends.
Here are the year-over-year changes from 1933-2018:
I labeled specific years with the highest year-over-year increases. 2020 will likely be about a 10% increase over 2018 deaths, and that is much higher than the highest spikes we see in the historical record.
(Obviously, if I had numbers going back to the Spanish flu, that would dwarf all the other mortality spikes.)
Some of the years, I have to dig to understand what’s going on (I’ve started looking at 1993, and I think there are a couple of trends intersecting there, with the predominant one being AIDS).
Two of the years, 1957 and 1968, I know exactly why they spiked.
Comparison of COVID-19 to 20th Century Flu Pandemics
Those were two flu pandemics — the “Asian flu” in 1957-1958 and the “Hong Kong flu” in 1968.
Those both had fairly large mortality results in the U.S. at the time.
The 1957-1958 flu pandemic killed about 116K Americans — if I scaled that to the current U.S. population, that would be about 216K dead. That’s about the same order of magnitude as COVID, if a little less.
The 1968 pandemic had less of an impact, at 100K U.S. deaths, which would scale up to about 161K deaths today, so not quite as bad, but pretty bad.
For COVID, there will be about a 10% (or a little higher) increase in the number of deaths from 2019 to 2020, given my current best estimate.
For the 1957 & 1968 boost, that was an increase of about 4.3% to 4.4%, even though scaled up, it’s about the same order of magnitude as COVID. That’s because the raw death rate was higher back then – in general, more people died at the same age. So higher proportional counts of deaths weren’t as large a step-up in mortality rates compared to the effect COVID-19 is having in 2020.
Let me compare the actual increases in death count by age group for each of these years, against my best estimate (not minimal projection) for 2020:
Look all the way to the right to see that, in percentage mortality increase terms, COVID-19 is showing a larger relative increase in death by over a factor of 2. The two prior pandemics saw years with about 4% increase in death counts, and 2020 will likely come in about 10% higher compared to 2018.
The age profiles are different in impact, with both the 1968 and 2020 pandemic years showing drops in deaths for children, with more impact on older age groups. The 1957 flu pandemic had a disproportionate effect on both children and old people, which is pretty common in seasonal flu impact as well.
Again, in a future post, I will look at single-year changes in mortality rates for age groups, as well as compare the base mortality for the groups between the years… and you will see that while these three pandemics had similar raw excess death rates, compared to the size of the population, our current population over 50 years later is more used to a much lower death rate.
So an infectious disease having a similar death impact in raw rate will be relatively harsher for us: we’re no longer used to a population of widespread smoking in which men usually had their first heart attack in their 50s. Even childhood mortality was much higher then than now.
That’s it for analysis on this post – below you will find my background materials, link to my spreadsheet and data sources, etc.
Some pieces on prior flu pandemics
Baltimore Sun, April 2020: Asian flu epidemic of 1957 killed over a million worldwide but only 65 in Baltimore
The National Interest, May 2020: The 1957 Pandemic Was a Lot Like Coronavirus—But It’s Also Different In Important Ways
The Daily Gazette, March 2020: Asian flu 1957: How the region coped with another pandemic (Capital Region of New York state)
WNYC, December 2013: The 1957 pandemic: Not the Flu We Knew
City Journal, March 2020: Say Your Prayers and Take Your Chances: Remembering the 1957 Asian flu pandemic
JSTOR Daily, April 2020: How America Brought the 1957 Influenza Pandemic to a Halt
Online MedEd, September 2020: The Forgotten History of the 1968 ‘Hong Kong Flu’ Pandemic
The Lancet, May 2020: Revisiting the 1957 and 1968 influenza pandemics
Background and methods
Back in April, I wrote about baseline mortality, looking at recent age structure of deaths as well as causes of death.
I decided to pull this perspective farther back, and just look at total deaths. My data come from The Human Mortality Database, which has historical mortality stats from all sorts of countries (my favorite is Sweden with data going back to 1676).
The U.S. data originally comes from the CDC, and I spot-checked death counts for specific years. In general, the old CDC publications are scanned-in typeset documents, and I’m happy the Human Mortality Database folks have made the transfer from the old docs.
I pulled the U.S. counts of deaths, which currently cover 1933 through 2018, and have breakouts by year, sex, and age, and they also group these in various blocks, for researchers looking at long-term mortality trends. Single year deviations generally aren’t of interest for those trying to determine how longevity might evolve, for example. However, I did use the single-year, single-age, single-sex extract. I did not compare the sex gap on mortality in this post, but may in a future post.
For 2020 mortality, I used the CDC’s age and sex breakout, and I solely used the “deaths from all causes” column for today’s analysis. Given some of the heightened mortality in the 35-44 bucket, I’m going to want to dig into those details more in the future — there may be excess deaths in this group due to secondary effects of COVID (drug overdoses, suicides, car accidents).
For my two 2020 projections,I did this two ways. For my “minimal” projection, I took the deaths from the week ending 2/1/2020 to 10/17/2020 (a 265-day period) and then “filled in” the remaining 101 days of 2020 with a proportional number of deaths from 2018. Essentially, I assumed no excess deaths in January 2020, and no excess deaths after 10/17/2020 (and also assumed that the death counts in October, for instance, wouldn’t increase). This is what I consider a lower bound estimate for 2020 deaths.
For my current best estimate, I took current total mortality estimates and projected them for the full year. I will likely adjust this estimate, because it may be a bit pessimistic given current case fatality trends for COVID, but it may also capture continuing economic hardship and especially social stress for people.
The current spreadsheet for this post can be downloaded from my DropBox. To keep versions controlled, I will not change that spreadsheet, and any future estimates will be in separate files and linked separately.
Enjoy!